This information is for men who have already had surgical removal of the prostate gland, and now they have been recommended to undergo radiation therapy.
Who needs radiation therapy after prostatectomy?
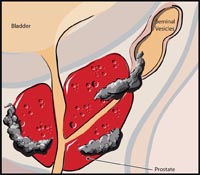 Sometimes prostate removal does not completely cure the cancer. Even if the surgeon has done an excellent / perfect surgery, and it looks like he got all the cancer, there can still sometimes be some cancer cells left behind. This is especially common if the cancer was breaking through the outer lining of the prostate gland and going into tissues around the prostate (see picture on right). It’s also more common when there was a lot of cancer found in the prostate gland. Radiation therapy after prostatectomy may be recommended in the following four situations:
Sometimes prostate removal does not completely cure the cancer. Even if the surgeon has done an excellent / perfect surgery, and it looks like he got all the cancer, there can still sometimes be some cancer cells left behind. This is especially common if the cancer was breaking through the outer lining of the prostate gland and going into tissues around the prostate (see picture on right). It’s also more common when there was a lot of cancer found in the prostate gland. Radiation therapy after prostatectomy may be recommended in the following four situations:
- The pathologist sees that cancer has broken through the prostate capsule (lining) and has gone into tissues surrounding the prostate. This is stage 3 cancer and includes cancer that has spread into the tissues around the prostate, the seminal vesicles, or in more advanced cases into the bladder, rectum, or lymph nodes.
- There are “positive surgical margins”. This means that cancer cells were right at the edge of the tissue that was removed by the surgeon, which means that cancer cells may still be inside the body.
- The PSA does not drop down to zero after surgery, especially in conjunction with #1 or #2.
- The PSA starts to climb again at some time after surgery.
Often there is a combination of these 4 factors present.
Timing of radiation therapy after prostatectomy
It is best to wait at least 3 months after surgery if possible before starting the radiation, in order to give a chance for full healing. It is good for the urinary control to be as good as it’s going to get before starting radiation. If additional healing time is needed, some hormone therapy can be used to be able to safely delay the radiation.
It is debatable when a patient should be referred for radiation. Some urologists prefer to wait until the PSA starts to rise again before referring the patient. This is also called salvage radiation. Other urologists will see some warning signs on the pathology report and will refer the patient early, before giving the cancer a chance to start growing back. This is also called adjuvant radiation.
How do we know where do we aim the radiation and how many treatments?
When we radiate after prostatectomy, we treat the tissues surrounding where the prostate gland used to be. This is known as the “prostate surgical bed”. The anatomy becomes a little odd, as the bladder and the rectum and the other surrounding tissues get pulled into the empty area where the prostate previously was. When we radiate, we end up treating a little more bladder and rectum than we typically do with normal prostate radiation. We have to use a slightly lower radiation dose because of this. We have found that a dose of about 39 treatments is the most we can safely give, instead of the 45 like we normally do when the prostate gland is still there. So our dose is typically 180 cGy daily for 39 days = 7020 cGy total, instead of the usual 8100 cGy. Other cancer centers may use higher or lower dosages than this.
When the PSA is rising after surgery it can be do to 3 possibilities:
- Some healthy prostate gland tissue was left behind and is making PSA
- Prostate cancer is recurring in the prostate surgical area
- Prostate cancer is recurring in the lymph nodes or the bones (metastatic cancer)
Generally, there is no way to know for sure which situation is occurring, but #2 is the most likely. When we give post-prostatectomy radiation we are playing the odds that the PSA is coming from cancer cells that are located in the tissues around where the prostate used to be. Scans are mostly useless to determine where the cancer is recurring, because when the PSA is very low the cancer will be too tiny to be seen on any scan.
Side effects
Because there is no prostate gland, often the urinary side effects are actually milder compared with men who still have their prostate gland. There can be some urgency, i.e. having to rush to the bathroom to urinate. There can be some increased leakage. The rectum can become irritated causing some looseness, mucous, and hemorrhoid irritation. These short term side effects usually clear up within 1 – 2 months after completing radiation. There is also the risk of long term (permanent) worsening of urine control, but this is not common. If you have been able to get erections since the surgery they may become further weakened by the radiation.
The success rate for radiation after surgery
Before proceeding with radiation you need to know that this treatment does not guarantee that you will be cured. It may be a very good idea and the best option, but it’s not a sure thing because:
- After surgery the area has a reduced blood supply, and cancer cells with less available oxygen may be more radiation resistant. In addition, we have to give a lower dose of radiation (39 treatments instead of 45) to limit the side effects. The aiming of radiation is also a little trickier, as there is no prostate gland to aim at.
- Some cancer cells may already be in the lymph nodes or bones. Even if scans are all clear, there can be small amounts of cancer in those areas that do not yet show up. The radiation does not treat the lymph nodes or bones. If there are any cancer cells there, tumors may develop in those area in the future.
So, cancer cells may survive radiation therapy inside the radiated area or outside the radiated area. There is an online calculator (google “MSKCC prostate nomogram”) which estimates the chance that you’ll still be cancer free 6 years after having the radiation. A typical result is 50 – 60%. Ask your doctor for help with this. If your PSA stays very low for 3 – 5 years after radiation then there is an excellent chance of long term success.
What happens if radiation after prostatectomy fails?
In that case there is no other treatment that can be used to try to cure the cancer. The main treatment becomes hormone therapy, to try to slow the cancer down. There is no rush to start on the hormone therapy. Hormone therapy can often keep the cancer under control for several years.
Q) How many people are totally cured after radiation after previous prostatectomy?
A) About 50%.
Q) What should the PSA drop to after treatment?
A) Ideally I would like to see it get down to 0.00 – 0.05 within 12 months after finishing radiation, but as long as it drops some and stabilizes that is encouraging.
Q) Do you ever radiate the lymph nodes as well?
A) Yes sometimes we radiate the pelvic lymph nodes. Especially if cancer has been found in the lymph nodes, and/or the Gleason score is 8 or above, and/or the cancer has spread into the seminal vesicles.
Q) Where does the PSA come from if I have no prostate gland?
A) PSA is produced by both normal prostate cells and by cancerous prostate cells. Since your prostate gland has been totally removed, it can only be cancerous prostate cells that are still making PSA. Even if these prostate cancer cells have metastasized to somewhere else in the body they will still produce PSA. The most likely spot for the cells to be is in the area where the prostate gland used to be.
